Your doctor says to avoid rice completely, your grandmother insists rotis are healthier, and nutrition articles contradict each other constantly. Confusion about rice vs roti for diabetics leaves you paralyzed, avoiding both and feeling deprived of cultural staples. Understanding glycemic index comparison plus implementing strategic carbs for diabetics creates sustainable blood sugar control while enjoying traditional Indian foods. This guide reveals how Indian diabetics can make informed choices about chapati vs rice for optimal metabolic health without cultural deprivation.
What Is Rice Vs Roti For Diabetics and Why Indian Dieters Should Care?
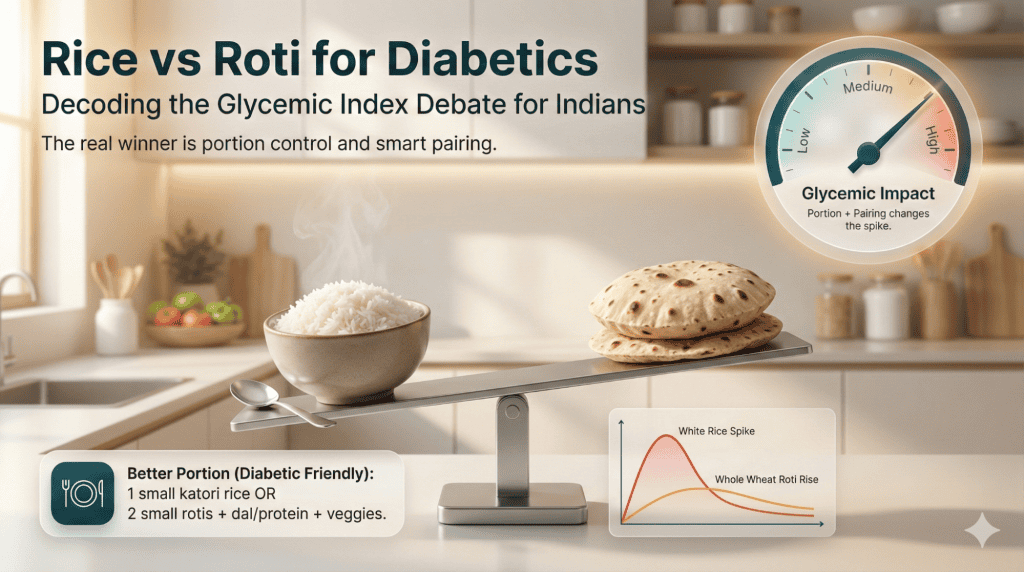
Rice vs roti for diabetics involves comparing blood sugar impact of India’s two staple carbohydrates through glycemic index comparison and portion control. White rice has glycemic index of 73 (high) while whole wheat roti scores 62 (medium), but actual blood sugar response depends on portion size, preparation method, and accompanying foods. Additionally, neither is inherently bad—strategic consumption of both supports carbs for diabetics management. Moreover, completely eliminating cultural staples creates unsustainability and social isolation. Therefore, understanding how to include Indian staples diabetes appropriately works better than complete avoidance.
Why Rice Matters for Indian Bodies
Indians need practical guidance on rice vs roti for diabetics given genetic predisposition to diabetes and cultural centrality of these foods. Additionally, Indians develop diabetes at younger ages and lower BMI than other populations making carb management crucial. Moreover, social and family meals revolve around rice or roti making complete elimination culturally unrealistic. Furthermore, chapati vs rice choice significantly impacts blood sugar control throughout the day. In fact, portion control and preparation methods matter more than choosing one over the other absolutely. Therefore, learning strategic consumption of Indian staples diabetes creates sustainable diabetes management.
Common Myths Debunked About This Topic
Let’s clear myths about rice vs roti for diabetics. First, roti isn’t always better—white wheat flour has similar glycemic impact as white rice. Second, completely avoiding rice isn’t necessary—portion control and pairing with protein/fiber works. Third, brown rice isn’t magical—it’s only slightly better than white requiring portion control still. Fourth, timing doesn’t eliminate impact—eating rice at lunch versus dinner doesn’t fundamentally change blood sugar response without portion control. Additionally, soaking or cooling rice doesn’t dramatically reduce glycemic impact despite internet claims. Finally, diabetes doesn’t mean never eating traditional foods—strategic consumption allows cultural participation. Therefore, nuanced approach beats absolute rules for carbs for diabetics.
The Science Behind Rice Vs Roti For Diabetics for Indians
How Rice Works in Your Body
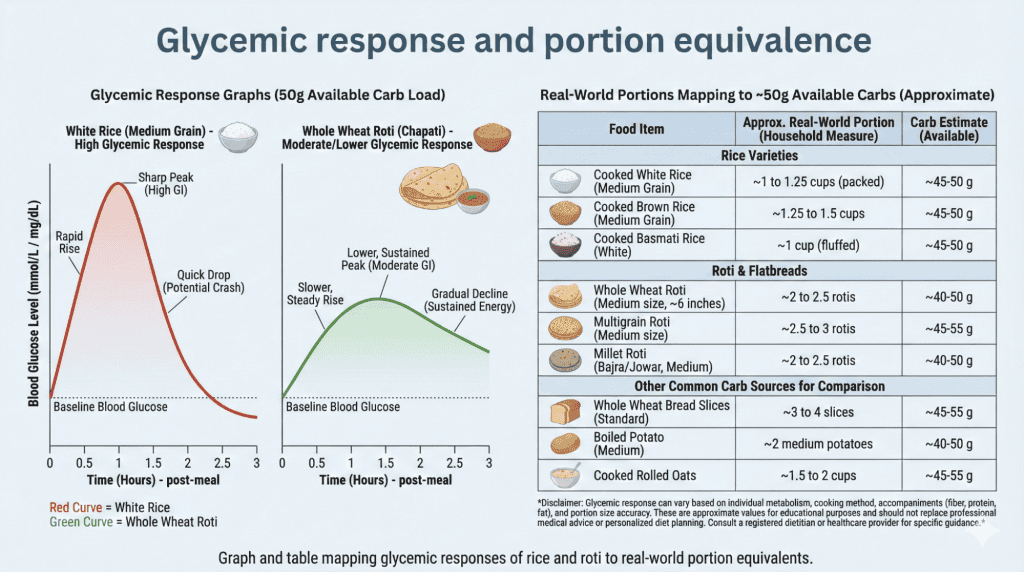
Carbs for diabetics affects blood sugar through digestion speed and glucose release into bloodstream. White rice digests rapidly causing sharp blood sugar spike within 30 minutes requiring significant insulin response. Additionally, whole wheat roti digests slower due to fiber content creating more gradual rise. Moreover, portion size matters tremendously—1 cup white rice (200g) raises blood sugar more than 2 small rotis (60g total). Furthermore, pairing rice or roti with protein, fat, and fiber slows digestion reducing glycemic impact by 30-40%. Therefore, glycemic index comparison provides guidance but real-world consumption includes multiple factors affecting actual blood sugar response.
The Connection Between Carbs For Diabetics and Health
Indian staples diabetes management affects comprehensive metabolic health beyond just blood sugar numbers. Uncontrolled blood sugar from excessive carbs for diabetics damages blood vessels, nerves, kidneys, and eyes over time. Additionally, frequent blood sugar spikes and crashes create energy fluctuations, increased hunger, and weight gain worsening insulin resistance. Moreover, appropriate carb consumption supports sustained energy, satiety, and metabolic function when portioned correctly. Furthermore, cultural food participation supports mental health and social connection crucial for long-term adherence. Therefore, strategic chapati vs rice choices support both physical and psychological wellbeing.
What Research Shows for Indian Population
Research on rice vs roti for diabetics in Indians reveals important practical findings. Studies show Indians consuming white rice as staple have 55% higher diabetes risk than those consuming whole grains primarily. Additionally, research demonstrates replacing white rice with brown rice or millets reduces diabetes risk by 16%. Moreover, studies indicate portion control matters more than rice versus roti choice—1 katori (100g cooked) of either works better than unlimited roti assumption. Furthermore, research shows Indians pairing carbs with protein and fiber reduce post-meal blood sugar by 35% compared to carbs alone. Therefore, evidence supports moderate portions of preferred grain with strategic meal composition for Indian staples diabetes management.
Glycemic Index Comparison: What to Watch For
Physical Signs and Symptoms to Monitor
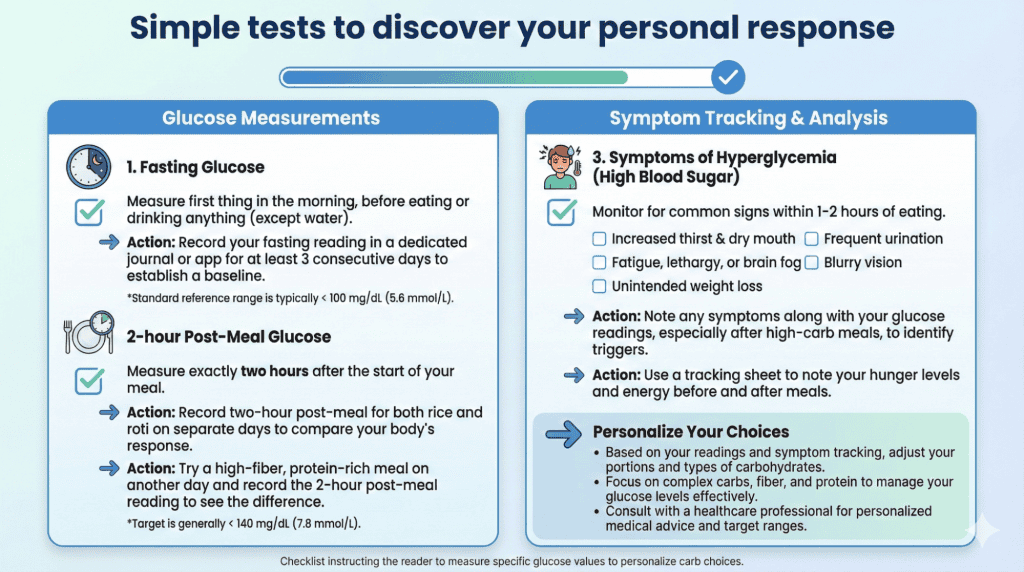
Glycemic index comparison effectiveness shows through blood sugar patterns and diabetes symptoms. Monitor fasting blood sugar staying below 100 mg/dL and post-meal readings below 140 mg/dL indicating good control. Additionally, HbA1c below 6.5% shows excellent 3-month average control from appropriate carbs for diabetics. Moreover, steady energy without mid-afternoon crashes suggests stable blood sugar from balanced meals. Furthermore, reduced thirst, frequent urination, and blurred vision indicate improving control. Watch for hypoglycemia symptoms including shakiness, sweating, or confusion suggesting overcorrection requiring adjustment. Therefore, multiple markers validate rice vs roti for diabetics strategy effectiveness.
Emotional and Mental Health Indicators
Indian staples diabetes management should reduce anxiety, not create food fear or social isolation. You should feel confident making carb choices at restaurants and family gatherings. Additionally, flexible approach allowing both rice and roti based on preference and situation supports mental wellbeing. Moreover, food relationship should feel balanced without extreme restriction or guilt after eating cultural foods. Furthermore, ability to participate in social and cultural events without anxiety about food validates sustainable approach. However, watch for obsessive carb counting or extreme food fear requiring professional support. Therefore, mental health stability indicates chapati vs rice strategy supports comprehensive wellbeing.
When to Consult a Healthcare Professional
Consult endocrinologists for diabetes diagnosis, medication adjustments, or uncontrolled blood sugar despite dietary efforts. Additionally, work with certified diabetes educators learning blood sugar monitoring, carb counting, and meal planning strategies. Moreover, see registered dietitians specializing in diabetes creating personalized meal plans incorporating preferred carbs for diabetics within control targets. Furthermore, if implementing rice vs roti for diabetics strategies consistently without blood sugar improvement, evaluation ensures no underlying issues preventing control. Therefore, professional guidance optimizes Indian staples diabetes management through individualized approaches.
Indian Lifestyle Factors Affecting Rice Vs Roti For Diabetics
Modern Indian Diet Challenges and Solutions
Modern Indian eating patterns challenge carbs for diabetics management through excessive portions and refined grains. Restaurant servings provide 2-3 cups rice (400-600g) when diabetics need 1/2-1 cup (100-200g). Additionally, many Indians eat unlimited rotis assuming they’re healthier than rice without portion awareness. Moreover, refined white rice and white wheat flour dominate over whole grain alternatives. Solutions include measuring portions using katori (1 small katori = 100g cooked rice or 2 small rotis), switching to brown rice or whole wheat alternatives when possible, and always pairing Indian staples diabetes with protein and vegetables. Therefore, strategic modifications support blood sugar control.
Work-Life Balance and Urban Living Impact
Urban professional lifestyle creates challenges for rice vs roti for diabetics management. Office lunches often include unlimited rice or rotis without portion control. Additionally, eating out provides limited whole grain options. Moreover, time constraints prevent meal preparation leading to reliance on refined carb-heavy convenience foods. Solutions include packing measured portions from home, requesting half-servings at restaurants, and choosing chapati vs rice options with protein and vegetables. Additionally, meal prep on weekends ensures appropriate portions readily available. Therefore, proactive planning supports glycemic index comparison strategy implementation.
Cultural and Social Influences on Health
Indian cultural factors affect Indian staples diabetes management through food-centered social events. Family gatherings pressure eating large portions refusing appearing rude. Additionally, hosts serve generous rice or roti portions assuming more shows care. Moreover, cultural perception that diabetes means never enjoying traditional foods creates isolation. Solutions include educating family about health needs, taking appropriate portions regardless of serving size, and focusing on vegetables and proteins at gatherings. Additionally, strategic planning allows small controlled portions of favorites maintaining cultural participation. Therefore, balancing culture with health makes carbs for diabetics sustainable.
Best Indian Foods for Rice Vs Roti For Diabetics Management
Traditional Indian Foods That Support Chapati Vs Rice
Strategic grain choices optimize rice vs roti for diabetics blood sugar control. Better options include brown rice (GI 68), whole wheat chapati (GI 62), or alternative grains like quinoa (GI 53), barley (GI 28), or millets (GI 50-55) providing lower glycemic impact. Additionally, always pair grains with protein from dal, paneer, eggs, or chicken slowing digestion and reducing blood sugar spike. Moreover, include generous non-starchy vegetables adding fiber and volume without significantly affecting blood sugar. Furthermore, healthy fats from nuts, seeds, or moderate oil improve satiety and slow carb absorption. Therefore, complete balanced meals support Indian staples diabetes management effectively.
Modern Indian Meal Options and Healthy Recipes
Create diabetic-friendly meals using carbs for diabetics strategically. Include measured grain portions: 1 small katori brown rice (100g cooked) or 2 small whole wheat rotis (30g each), substantial protein from 1 katori dal plus 100g paneer or chicken, generous vegetables filling half the plate providing fiber and nutrients, and small amount healthy fat from nuts or moderate oil. Additionally, choose lower glycemic alternatives like bajra, jowar, or ragi rotis when possible. Moreover, prepare rice with vegetables (vegetable pulao) or dal (khichdi) naturally limiting portions while adding nutrition. Therefore, balanced composition supports glycemic index comparison goals.
Foods to Limit or Avoid for Better Results
Certain preparations worsen rice vs roti for diabetics blood sugar impact. White rice in large portions (2+ cups) causes severe spikes requiring significant insulin or medication. Additionally, fried rice or biryani with added fats and oils increase calories without improving glycemic response. Moreover, refined white flour products like naan, paratha, or puri have similar impact to white rice despite different form. Furthermore, rice-based sweets or desserts combine high glycemic carbs with sugar creating extreme blood sugar elevation. Fruit juices even without added sugar spike blood sugar rapidly unlike whole fruits. Therefore, limiting these allows room for appropriate portions of preferred Indian staples diabetes within control targets.
Portion Sizes and Meal Timing for Indians
Strategic portions optimize chapati vs rice consumption for diabetics. Use hand measures: 1 fist-size portion cooked rice (approximately 1 small katori or 100g) or 2 small rotis (each size of palm or 30g). Additionally, make lunch largest meal when insulin sensitivity peaks and dinner smaller controlling evening blood sugar. Moreover, spacing meals 4-5 hours apart prevents grazing and allows blood sugar normalization between eating. Furthermore, eating protein and vegetables before carbs slows digestion reducing glycemic impact by 30%. Include adequate fiber 25-30g daily from vegetables and dal supporting blood sugar control. Therefore, strategic timing and portions support carbs for diabetics management.
Lifestyle Changes to Support Rice Vs Roti For Diabetics
Indian Staples Diabetes: The Right Approach for Indians
Implementing sustainable Indian staples diabetes management requires flexible evidence-based approach. Both rice and roti can fit diabetic meal plans with appropriate portions and pairings. Additionally, choose whole grain versions when possible but don’t eliminate white rice/wheat completely if that creates adherence issues. Moreover, focus on overall meal composition: protein, vegetables, and controlled grain portions matter more than rice versus roti debate. Furthermore, monitor blood sugar responses to your specific choices as individual variation exists. Some diabetics handle rice better, others rotis—personal testing reveals what works for your body. Therefore, individualized flexible approach beats rigid rules.
Sleep and Stress Management Strategies
Sleep and stress affect carbs for diabetics metabolism and blood sugar control. Inadequate sleep increases insulin resistance by 30% making blood sugar harder to control despite perfect diet. Additionally, chronic stress elevates cortisol raising blood sugar and promoting abdominal fat storage. Moreover, poor sleep increases hunger and cravings for high-glycemic carbs worsening control. Solutions include prioritizing 7-8 hours quality sleep, establishing stress management through meditation or yoga, and recognizing rice vs roti for diabetics choices work optimally when lifestyle supports metabolic health. Therefore, comprehensive approach beyond just food supports diabetes management.
Daily Habits That Make a Real Difference
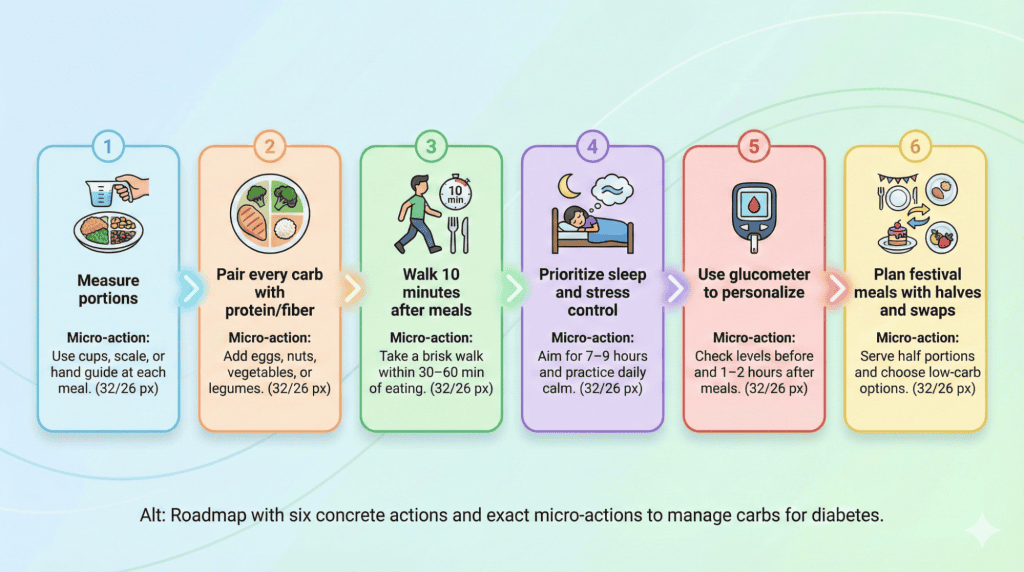
Small consistent habits optimize glycemic index comparison strategy long-term. Monitor blood sugar regularly tracking how different foods and portions affect your individual response. Additionally, measure grain portions consistently using katori or cups preventing portion creep over time. Moreover, track meals and blood sugar in journal or app revealing patterns guiding choices. Furthermore, walk 10-15 minutes after meals reducing post-meal blood sugar by 15-20% regardless of rice or roti choice. Include strength training 2-3 times weekly improving insulin sensitivity supporting better Indian staples diabetes control. Therefore, daily habits create environment supporting blood sugar management.
Your 7-Day Rice Vs Roti For Diabetics Management Meal Plan
| Day | Breakfast | Lunch | Evening Snack | Dinner |
| Day 1 | Vegetable poha (1 katori) + egg + curd | Brown rice (1 katori) + dal + chicken curry + vegetables + salad | Roasted chana + cucumber | 2 small whole wheat rotis + dal + vegetables + raita |
| Day 2 | Moong dal cheela (2) + paneer + vegetables | 2 small bajra rotis + dal + fish curry + vegetables | Nuts + apple slices | Brown rice (1 katori) + dal + mixed vegetables + curd |
| Day 3 | Oats (1 katori) + milk + nuts + berries | Brown rice (1 katori) + sambhar + egg curry + vegetables | Buttermilk + roasted makhana | 2 small whole wheat rotis + dal + leafy greens + raita |
| Day 4 | Vegetable upma (1 katori) + boiled eggs + curd | 2 small ragi rotis + dal + chicken curry + vegetables + salad | Curd + cucumber + seeds | Brown rice (1 katori) + dal + vegetables + raita |
| Day 5 | Idli (3) + sambhar + egg bhurji + chutney | Brown rice (1 katori) + dal + paneer curry + vegetables | Roasted chana + carrot sticks | 2 small jowar rotis + dal + mixed vegetables + curd |
| Day 6 | Besan cheela (2) + vegetables + curd + nuts | 2 small whole wheat rotis + dal + fish curry + vegetables + salad | Nuts + seasonal fruit | Brown rice (1 katori) + dal + vegetables + raita |
| Day 7 | Vegetable daliya (1 katori) + boiled eggs + milk | Brown rice (1 katori) + dal + chicken curry + vegetables | Buttermilk + roasted chana | 2 small bajra rotis + dal + leafy greens + raita |
Note: Each day demonstrates both rice vs roti for diabetics can fit with proper portions: 1 small katori brown rice (100g cooked) OR 2 small rotis (30g each). Always paired with adequate protein (dal plus paneer/eggs/chicken/fish) and generous vegetables. Alternating grains provides variety while maintaining blood sugar control through portion awareness essential for Indian staples diabetes management.
Common Mistakes Indians Make with Rice Vs Roti For Diabetics
Diet Mistakes That Sabotage Progress
Biggest mistake is eating unlimited rotis assuming they’re “free” foods when they impact blood sugar similarly to rice in excessive amounts. Additionally, choosing white rice or white wheat flour thinking minimal difference when whole grains provide significant fiber benefit. Moreover, eating carbs alone without protein or vegetables causes rapid blood sugar spikes. Furthermore, not measuring portions allowing gradual increase from 1 katori to 2-3 over time. Completely eliminating rice or roti creates deprivation leading to eventual overconsumption. Therefore, measured portions of preferred carbs for diabetics with strategic meal composition works better than extreme restriction.
Lifestyle Pitfalls to Watch Out For
Many sabotage rice vs roti for diabetics efforts through implementation errors. Not monitoring blood sugar regularly prevents knowing how specific foods and portions affect individual response. Additionally, eating out without requesting smaller portions or half-servings. Moreover, family-style serving encouraging multiple helpings rather than single measured portion. Furthermore, not walking after meals missing simple intervention reducing blood sugar by 15-20%. Inadequate sleep and stress management undermine dietary efforts through insulin resistance. Therefore, comprehensive lifestyle approach supports glycemic index comparison strategy effectiveness.
How to Course-Correct When Things Go Wrong
If blood sugar remains uncontrolled despite implementing Indian staples diabetes strategies, troubleshoot systematically. Verify actual portions by weighing/measuring for one week as estimation often underestimates. Additionally, ensure pairing carbs with adequate protein and vegetables every meal not sometimes. Moreover, check if stress, inadequate sleep, or medications affect control requiring adjustment. Furthermore, monitor blood sugar 2 hours post-meal revealing which specific foods or portions cause problems for your individual response. If all factors optimized without improvement, medication adjustment may be necessary. Therefore, systematic approach identifies whether implementation or medical issues prevent chapati vs rice strategy success.
Frequently Asked Questions
Q1: What is rice vs roti for diabetics and how does it affect Indians?
Rice vs roti for diabetics involves comparing blood sugar impact: white rice (GI 73) versus whole wheat roti (GI 62) with actual response depending on portion size, preparation, and accompaniments more than inherent superiority. Indians particularly need practical guidance given genetic diabetes predisposition and cultural centrality of both foods making complete elimination unrealistic requiring strategic carbs for diabetics consumption instead.
Q2: What are the main signs of rice issues?
Signs include blood sugar above 140 mg/dL two hours after rice-containing meals, extreme energy crashes 1-2 hours after eating, increased thirst and frequent urination after carb-heavy meals, difficulty losing weight despite controlling calories, and HbA1c above 6.5% indicating poor 3-month control. Multiple indicators together suggest need for better portion control and glycemic index comparison strategy implementation.
Q3: What foods should Indians eat for better rice vs roti for diabetics?
Choose whole grain options: brown rice (GI 68), whole wheat chapati (GI 62), or lower alternatives like millets (GI 50-55), quinoa (GI 53), or barley (GI 28). Limit portions to 1 small katori rice (100g cooked) OR 2 small rotis (30g each), always paired with protein from dal plus paneer/eggs/chicken and generous non-starchy vegetables supporting Indian staples diabetes control.
Q4: Can rice be managed naturally?
Yes through strategic portion control limiting to 1 small katori brown rice (100g cooked) daily, pairing with protein and vegetables reducing glycemic impact by 30-40%, choosing whole grain versions when possible, walking 10-15 minutes after meals lowering post-meal blood sugar by 15-20%, and monitoring individual response adjusting based on personal blood sugar patterns for carbs for diabetics optimization.
Q5: How long does it take to see results with rice vs roti for diabetics changes?
Blood sugar improvements appear within 3-7 days of implementing proper portions and meal composition. HbA1c reflecting 3-month average improves within 8-12 weeks of consistent Indian staples diabetes management. Weight loss and energy improvements become noticeable at 4-8 weeks. Long-term diabetes control requires sustained lifestyle changes maintaining appropriate chapati vs rice portions and pairings indefinitely.
Conclusion
Rice vs roti for diabetics reveals both can fit diabetic meal plans with strategic portions: 1 small katori brown rice (100g) OR 2 small whole wheat rotis (30g each) paired with protein and vegetables. For Indians, glycemic index comparison shows whole grains provide slight advantage but portion control matters more than choosing one exclusively. Understanding carbs for diabetics allows cultural food participation through measured consumption rather than complete elimination creating deprivation. Indian staples diabetes management succeeds through flexibility based on individual blood sugar response, preferences, and social context. Managing rice and roti isn’t about perfection—it’s about consistent appropriate portions with strategic meal composition supporting blood sugar control.
Start this week by measuring your current grain portions discovering actual consumption versus assumed amounts. Additionally, switch to brown rice or whole wheat rotis when possible for fiber benefit. Pair every carb-containing meal with protein and vegetables reducing glycemic impact by 30-40%.