You feel tired constantly despite sleeping enough. Sugar cravings hit hard mid-afternoon. Your belly fat won’t budge despite diet efforts. Blood tests show borderline high sugar levels. Your doctor mentioned “prediabetes” or “insulin resistance.” These signals indicate your body struggles managing blood sugar and insulin, affecting millions of Indians. An insulin balancing diet addresses root causes of weight gain, diabetes risk, and energy crashes. Understanding insulin resistance diet principles and implementing blood sugar control strategies transforms health outcomes. This guide reveals how Indians can optimize insulin function through strategic nutrition, preventing progression to diabetes while supporting sustainable weight loss.
What Is Insulin Balancing Diet and Why Indian Dieters Should Care?
Insulin balancing diet focuses on eating patterns maintaining stable blood sugar and insulin levels throughout the day. Insulin is hormone produced by pancreas that helps cells absorb glucose from blood for energy. Additionally, insulin resistance occurs when cells become less responsive to insulin, requiring higher amounts to achieve same effect. Moreover, chronically elevated insulin promotes fat storage, prevents fat burning, and eventually leads to type 2 diabetes. Therefore, blood sugar control through strategic food choices, meal timing, and lifestyle factors becomes essential for preventing disease and supporting weight management.
Why Insulin Matters for Indian Bodies
Indians face particularly high insulin resistance risk due to genetic predisposition and dietary patterns. Research shows Indians develop insulin resistance and diabetes at younger ages and lower BMI than other populations. Additionally, traditional high-carb diets centered on rice and rotis without adequate protein or fiber spike blood sugar repeatedly. Moreover, urban sedentary lifestyles worsen insulin sensitivity. Furthermore, abdominal fat accumulation common among Indians both causes and results from insulin resistance creating vicious cycles. In fact, prediabetes diet interventions become crucial as Indians progress from normal to diabetic faster than other populations. Therefore, understanding glucose stability through nutrition offers powerful disease prevention and reversal tool.
Common Myths Debunked About This Topic
Let’s clear up myths about insulin balancing diet. First, you don’t need to eliminate all carbs. Strategic carb selection and timing work better than extreme restriction. Second, fat doesn’t cause insulin resistance despite old beliefs. Sugar and refined carbs are primary drivers. Third, insulin resistance isn’t permanent or irreversible. Nutrition and lifestyle changes significantly improve insulin sensitivity. Fourth, you don’t need expensive supplements or special foods. Whole foods and strategic eating patterns work effectively. Additionally, checking blood sugar doesn’t require diabetes diagnosis. Monitoring helps anyone optimize insulin function. Finally, blood sugar control benefits everyone, not just diabetics or prediabetics. Stable glucose improves energy, mood, and weight management for all. Therefore, these strategies support comprehensive health beyond just disease prevention.
The Science Behind Insulin Balancing Diet for Indians
How Insulin Works in Your Body
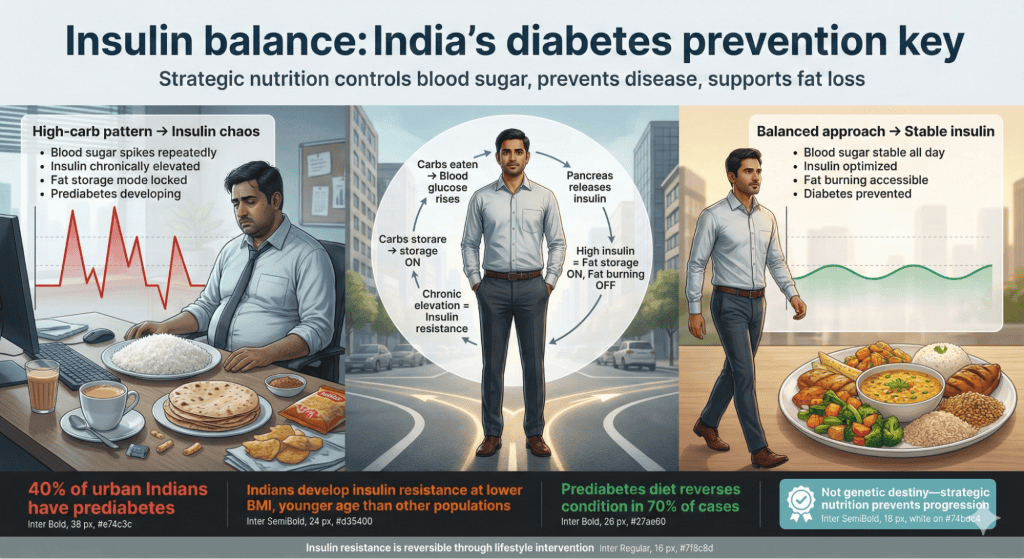
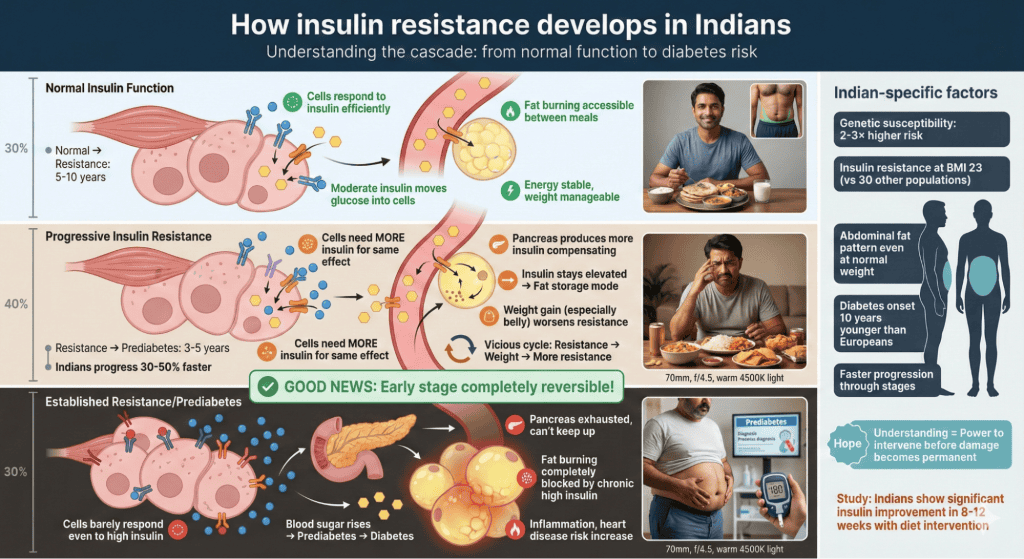
Insulin functions as master metabolic regulator affecting fat storage, hunger, and energy. When you eat carbs, blood sugar rises triggering insulin release to shuttle glucose into cells. Additionally, insulin promotes fat storage and prevents fat burning while elevated. Moreover, frequent blood sugar spikes from refined carbs keep insulin chronically high preventing fat loss. Furthermore, over time cells become resistant requiring more insulin achieving same effect, creating insulin resistance. This leads to weight gain, particularly belly fat, increased hunger, energy crashes, and eventually prediabetes or diabetes. In fact, insulin sensitivity determines how efficiently your body uses carbs for energy versus storing them as fat. Therefore, improving insulin function through insulin balancing diet creates metabolic environment supporting fat loss and disease prevention.
The Connection Between Insulin Resistance Diet and Health
Insulin resistance diet affects multiple health markers beyond just blood sugar. Improving insulin sensitivity reduces inflammation throughout body, root cause of most chronic diseases. Additionally, better blood sugar control stabilizes energy levels eliminating crashes and cravings. Moreover, lower insulin allows body to access fat stores for energy supporting weight loss. Furthermore, reducing insulin resistance decreases risk of heart disease, stroke, Alzheimer’s, PCOS, and certain cancers. Better glucose regulation improves fertility, skin health, and mood stability. In fact, prediabetes diet interventions reverse prediabetes in up to 70% of cases preventing diabetes development. Therefore, strategic nutrition addressing insulin resistance creates comprehensive health improvements extending far beyond preventing one disease.
What Research Shows for Indian Population
Research on insulin resistance in Indians reveals alarming prevalence and unique patterns. Studies show Indians have insulin resistance rates 2-3 times higher than other populations at same BMI. One study found 40% of urban Indians have prediabetes with many unaware. Additionally, research demonstrates Indians develop diabetes 10 years younger on average than Europeans. Moreover, studies show insulin balancing diet interventions emphasizing protein, fiber, and reduced refined carbs significantly improve insulin sensitivity in Indians within 8-12 weeks. Furthermore, research indicates Indians need lower carb intakes than current consumption for optimal glucose stability due to genetic susceptibility. In fact, studies suggest aggressive lifestyle intervention is more effective than medication alone for prediabetes reversal in Indians. Therefore, nutritional approaches become first-line treatment for insulin resistance.
Insulin Resistance: What to Watch For
Physical Signs and Symptoms to Monitor
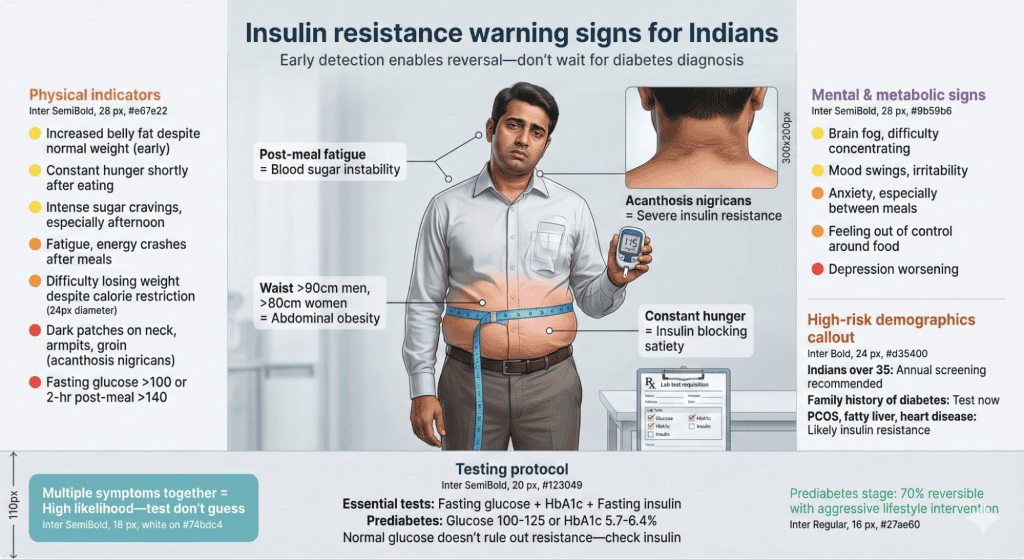
Insulin resistance creates observable symptoms before blood tests show problems. Increased abdominal fat despite overall weight being normal indicates insulin issues. Additionally, dark patches on neck, armpits, or groin called acanthosis nigricans signal severe insulin resistance. Moreover, constant hunger shortly after eating and intense sugar cravings indicate blood sugar instability. Fatigue and energy crashes, especially after carb-heavy meals, suggest poor glucose stability. Furthermore, difficulty losing weight despite calorie restriction indicates insulin blocking fat burning. Watch for these signs. Regular blood sugar monitoring showing levels above 100 fasting or above 140 two hours post-meal confirms problems. In fact, experiencing several symptoms together strongly suggests insulin resistance requiring dietary intervention even before formal diagnosis.
Emotional and Mental Health Indicators
Insulin and blood sugar control profoundly affect mental health and cognitive function. Brain fog and difficulty concentrating often stem from blood sugar instability and insulin resistance. Additionally, mood swings, irritability, and anxiety worsen with glucose crashes. Moreover, depression correlates with insulin resistance through inflammatory pathways and neurotransmitter disruption. Furthermore, intense food cravings and feeling out of control around food often relate to blood sugar instability, not just willpower. Some people experience anxiety or shakiness between meals from reactive hypoglycemia. In fact, many mental health symptoms improve dramatically when blood sugar stabilizes through insulin balancing diet, sometimes more than psychiatric medications alone achieve. Therefore, addressing insulin function supports mental health alongside physical health.
When to Consult a Healthcare Professional
Get tested if experiencing symptoms suggesting insulin resistance: persistent fatigue, difficulty losing weight, increased belly fat, dark skin patches, or family history of diabetes. Request fasting glucose, HbA1c, and ideally fasting insulin tests for comprehensive assessment. Additionally, if diagnosed with prediabetes, work with doctors and dietitians creating aggressive intervention plan as prediabetes diet changes can reverse condition. Moreover, if you have PCOS, fatty liver, or cardiovascular disease, insulin resistance likely contributes requiring specific treatment. Furthermore, annual testing makes sense for Indians over 35 given high population risk. If implementing insulin resistance diet independently for 3 months without blood sugar or symptom improvement, medical evaluation ensures no other underlying conditions. Therefore, medical partnership supports optimal outcomes.
Indian Lifestyle Factors Affecting Insulin Balancing Diet
Modern Indian Diet Challenges and Solutions
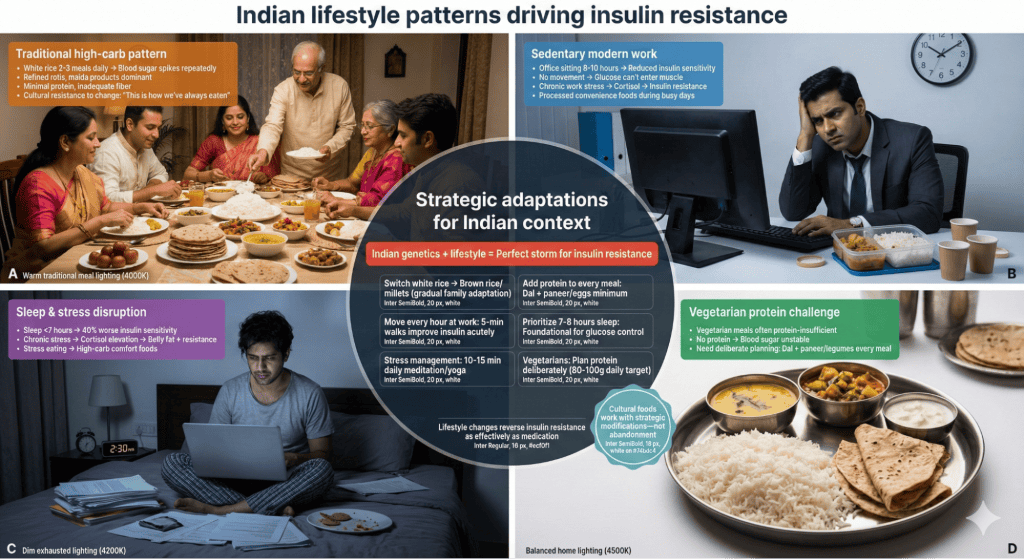
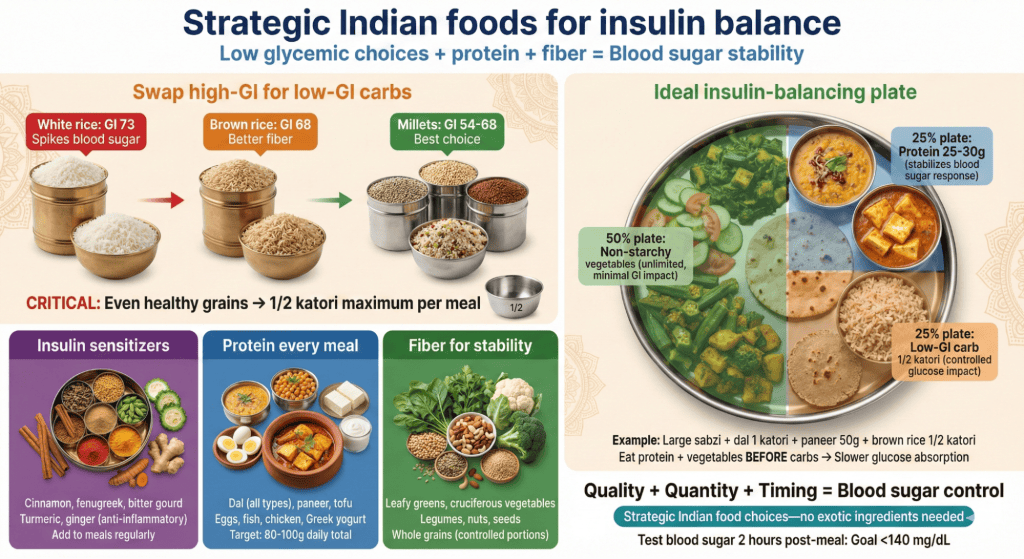
Traditional and modern Indian eating patterns create perfect conditions for insulin resistance through excessive refined carbs. White rice consumed 2-3 times daily spikes blood sugar repeatedly. Additionally, refined wheat rotis, maida products, and sugary snacks dominate modern diets. Moreover, inadequate protein and healthy fats fail to slow carb absorption. Furthermore, fruit juice, sweetened beverages, and chai with sugar add liquid sugar bypassing satiety mechanisms. Solutions include switching to brown rice, millets, or quinoa for lower glycemic impact. Additionally, pair all carbs with protein and fiber slowing absorption. Moreover, eliminate sugary drinks completely and minimize added sugar. Include adequate protein at every meal stabilizing blood sugar. Therefore, strategic modifications to familiar foods improve glucose stability without abandoning cultural cuisine.
Work-Life Balance and Urban Living Impact
Urban Indian lifestyle worsens insulin resistance through multiple mechanisms. Sedentary office work reduces insulin sensitivity as movement improves glucose uptake. Additionally, high stress elevates cortisol increasing blood sugar and promoting insulin resistance. Moreover, inadequate sleep impairs glucose metabolism and insulin function significantly. Furthermore, irregular eating patterns and reliance on processed convenience foods create blood sugar chaos. Solutions include moving every hour at work improving insulin sensitivity acutely. Additionally, prioritize 7-8 hours sleep as foundational for blood sugar control. Moreover, practice stress management actively as chronic stress sabotages metabolic health. Furthermore, meal prep ensuring regular balanced eating prevents desperate poor choices. Therefore, comprehensive lifestyle approach addresses insulin resistance more effectively than nutrition alone.
Cultural and Social Influences on Health
Indian cultural factors both help and hinder insulin balancing diet implementation. Food-centered celebrations and social obligations make refusing carb-heavy foods socially awkward. Additionally, generational beliefs that more food equals better health create resistance to portion control. Moreover, vegetarian diets require deliberate planning ensuring adequate protein for blood sugar stability. Furthermore, cultural preference for white rice over brown creates barriers despite health benefits. Solutions include educating family about diabetes prevention importance gaining support for dietary changes. Additionally, bring protein-rich options to gatherings ensuring something appropriate available. Moreover, gradually introduce whole grains at home allowing taste adaptation. Furthermore, reframe portion control as health-supporting, not restrictive. Therefore, culturally-sensitive approaches balance health needs with social realities.
Best Indian Foods for Insulin Balancing Diet Management
Traditional Indian Foods That Support Insulin Sensitivity
Strategic Indian food choices support insulin sensitivity naturally. Whole moong dal, chana dal, masoor dal provide protein and fiber stabilizing blood sugar. Additionally, non-starchy vegetables like cauliflower, beans, spinach, and methi have minimal glycemic impact. Moreover, nuts and seeds provide healthy fats and protein supporting glucose stability. Furthermore, whole grains like brown rice, bajra, jowar, ragi, and quinoa in moderation provide fiber slowing glucose absorption. Cinnamon, fenugreek, and bitter gourd have compounds improving insulin function. In fact, traditional Indian spices like turmeric and ginger reduce inflammation supporting insulin sensitivity. Therefore, emphasizing these foods while reducing refined carbs and sugar creates insulin balancing diet using familiar ingredients.
Modern Indian Meal Options and Healthy Recipes
Create meals optimizing blood sugar control using Indian foods. Breakfast needs substantial protein preventing morning glucose spike: moong dal cheela with vegetables, eggs, or paneer provides 25-30 grams protein. Additionally, lunch should include generous dal, moderate whole grain, plenty of vegetables, and raita stabilizing afternoon blood sugar. Moreover, dinner could emphasize protein and vegetables with minimal grain preventing nighttime glucose elevation. Include snacks combining protein and fiber: nuts with fruit, curd with seeds, or roasted chana maintaining stable glucose between meals. Furthermore, if eating rice, choose brown rice in small portions (1/2 katori) with plenty of vegetables and protein. These strategic meal compositions prevent blood sugar spikes while maintaining cultural food preferences. Therefore, balanced approach works better than extreme restriction.
Foods to Limit or Avoid for Better Results
Certain foods dramatically worsen insulin resistance requiring strict limitation. White rice, white bread, and maida products spike blood sugar rapidly. Additionally, sugary drinks including fruit juice, sodas, and sweetened chai provide liquid sugar overwhelming insulin response. Moreover, sweets, pastries, and processed snacks combine sugar and refined flour creating worst glycemic impact. Furthermore, fried foods often pair refined carbs with unhealthy fats promoting insulin resistance. Excessive alcohol impairs blood sugar control and liver function. In fact, even “healthy” foods like dried fruits, smoothies, or granola can spike blood sugar when portions are large or eaten alone without protein or fat. Therefore, minimize these foods while emphasizing whole foods, protein, fiber, and healthy fats supporting glucose stability.
Portion Sizes and Meal Timing for Indians
Strategic portions and timing optimize insulin balancing diet effectiveness. Limit grains to 1/2 katori brown rice or 1-2 small rotis per meal preventing glucose overload. Additionally, fill half plate with non-starchy vegetables providing volume without blood sugar impact. Moreover, include palm-size protein at each meal (20-30 grams) stabilizing glucose response to any carbs consumed. Space meals 4-5 hours apart allowing insulin to drop between eating episodes. Furthermore, avoid grazing or constant snacking keeping insulin elevated continuously. If snacking needed, choose protein and fat combinations rather than carbs alone. In fact, eating larger breakfast and lunch with lighter dinner aligns with circadian insulin sensitivity patterns. Therefore, appropriate portions and timing create metabolic environment supporting insulin function and fat loss.
Lifestyle Changes to Support Insulin Balancing Diet
Prediabetes Diet: The Right Approach for Indians
Addressing prediabetes aggressively prevents diabetes development in most cases through prediabetes diet intervention. Reduce total carbs to 40-45% of calories rather than typical 60-70% Indian intake. Additionally, increase protein to 25-30% supporting muscle which improves insulin sensitivity. Moreover, include healthy fats 25-30% providing satiety and supporting hormone function. Calculate appropriate calorie intake for modest weight loss as 5-10% weight reduction dramatically improves insulin sensitivity. Furthermore, emphasize low glycemic foods: non-starchy vegetables, legumes, nuts, seeds, whole grains in moderation. Monitor blood sugar regularly noticing how different foods affect your individual response. In fact, weight loss combined with insulin resistance diet reverses prediabetes in 70% of cases preventing diabetes. Therefore, aggressive early intervention creates dramatic outcomes.
Sleep and Stress Management Strategies
Sleep and stress management profoundly affect insulin sensitivity and blood sugar control. Inadequate sleep (less than 7 hours) increases insulin resistance and glucose intolerance significantly. Additionally, sleep deprivation increases hunger hormones and cravings for sugar and refined carbs. Moreover, chronic stress elevates cortisol promoting insulin resistance and abdominal fat accumulation. Furthermore, stress often triggers emotional eating of comfort foods worsening blood sugar. Solutions include prioritizing 7-8 hours quality sleep as non-negotiable for metabolic health. Additionally, practice daily stress management: meditation, yoga, walking, or hobbies for 10-15 minutes minimum. Furthermore, address underlying stress sources when possible rather than just managing symptoms. In fact, improving sleep and reducing stress often improves insulin sensitivity as much as dietary changes alone. Therefore, comprehensive approach addressing all factors creates optimal outcomes.
Daily Habits That Make a Real Difference
Small consistent actions support glucose stability long-term. Move after meals, even 10-15 minute walks significantly improve post-meal blood sugar. Additionally, drink water before meals improving satiety and preventing overeating. Moreover, eat protein and vegetables before carbs at meals slowing glucose absorption. Furthermore, monitor blood sugar periodically noting how different foods affect your response personalizing approach. Keep food diary tracking meals, blood sugar, energy, and symptoms identifying patterns. In fact, build muscle through strength training 2-3 times weekly as muscle is primary glucose disposal site improving insulin sensitivity. Additionally, manage portions using smaller plates and measuring grains preventing unconscious overeating. Therefore, these habits compound into significant insulin function improvement and diabetes prevention.
Your 7-Day Insulin Balancing Diet Management Meal Plan
This meal plan emphasizes protein, fiber, low glycemic foods for blood sugar control:
| Day | Breakfast (25-30g protein) | Lunch (30g protein, low GI) | Snack | Dinner (25g protein, minimal carbs) |
| Day 1 | Moong dal cheela (2) + paneer (50g) + vegetables + curd | Brown rice (1/2 katori) + dal (1 katori) + fish/paneer (100g) + vegetables + salad | Almonds (10) + apple | Grilled chicken/paneer + large vegetable salad + dal + raita |
| Day 2 | 2 boiled eggs + bajra roti + avocado + milk | Quinoa (1/2 bowl) + dal + palak paneer (100g) + vegetables | Roasted chana (1 bowl) | Fish/tofu + mixed vegetables + small brown rice (1/4 katori) |
| Day 3 | Besan cheela + vegetables + paneer + curd | Millets (1/2 katori) + dal + chicken curry (100g) + salad | Greek yogurt with nuts | Grilled fish/paneer + vegetable soup + leafy greens |
| Day 4 | Oats with milk + almonds + chia seeds + egg | Brown rice (1/2 katori) + rajma + vegetables + raita | Cucumber with hummus | Grilled protein + large mixed salad + dal |
| Day 5 | Vegetable poha + peanuts + 2 eggs + milk | Quinoa + dal + fish/paneer tikka + vegetables | Handful of walnuts | Chicken/paneer + stir-fried vegetables + small millet roti |
| Day 6 | Idli (2) + sambhar + 2 eggs + coconut chutney | Brown rice (1/2 katori) + dal + chicken (100g) + vegetables | Sprout salad | Grilled fish/tofu + vegetable soup + salad |
| Day 7 | Moong dal dosa (2) + paneer filling + curd | Millets (1/2 katori) + dal + mixed vegetables + paneer | Nuts + low GI fruit | Large mixed salad + grilled protein + dal |
Note: All meals emphasize protein (80-100g daily), fiber, low glycemic carbs in controlled portions. Non-starchy vegetables unlimited. Grains limited to 1/2 katori per meal. Test blood sugar 2 hours post-meal ensuring below 140 mg/dL.
Common Mistakes Indians Make with Insulin Balancing Diet
Diet Mistakes That Sabotage Progress
Biggest mistake is eating excessive carbs even from whole grains overwhelming insulin despite being “healthy.” Another error is eliminating all carbs creating unsustainability and metabolic slowdown. Additionally, many focus on reducing fat while keeping high carb intake, ineffective for insulin resistance. Moreover, drinking fruit juice or smoothies thinking they’re healthy when liquid sugar spikes insulin dramatically. Furthermore, not eating adequate protein fails to stabilize blood sugar or preserve muscle. In fact, eating tiny portions of everything including protein prevents satiety, leading to overeating carbs later. Therefore, strategic macronutrient balance with appropriate carb quality and quantity beats generic “healthy eating.”
Lifestyle Pitfalls to Watch Out For
Many sabotage insulin sensitivity through lifestyle choices. Sedentary lifestyle prevents glucose disposal into muscle maintaining high blood sugar. Additionally, chronic stress unchecked keeps cortisol elevated promoting insulin resistance. Moreover, inadequate sleep disrupts glucose metabolism regardless of perfect nutrition. Furthermore, not monitoring blood sugar means flying blind without feedback on what works. Continuing medications without reassessing need as insulin improves with lifestyle changes sometimes causes hypoglycemia. In fact, yo-yo dieting and weight cycling worsen insulin resistance over time. Therefore, consistent lifestyle alongside nutrition creates lasting insulin function improvement.
How to Course-Correct When Things Go Wrong
If implementing insulin balancing diet without blood sugar improvement after 8-12 weeks, troubleshoot systematically. Track actual carb intake verifying it’s truly reduced, not just perceived reduction. Additionally, check protein adequacy ensuring 80-100 grams daily. Moreover, verify sleep quantity and quality addressing if inadequate. Furthermore, assess stress levels implementing active management if high. Test blood sugar before and 2 hours after meals identifying specific problem foods. In fact, if lifestyle changes aren’t working, medical evaluation rules out other issues like thyroid dysfunction affecting glucose metabolism. Work with diabetes educator or dietitian personalizing approach if self-directed efforts insufficient. Therefore, systematic assessment identifies barriers preventing success.
Frequently Asked Questions
Q1: What is insulin balancing diet and how does it affect Indians?
Insulin balancing diet emphasizes foods maintaining stable blood sugar and insulin levels through protein, fiber, healthy fats, and controlled low-glycemic carbs. Indians face 2-3 times higher insulin resistance rates than other populations due to genetic susceptibility, requiring dietary strategies preventing progression to diabetes affecting 40% of urban Indians with prediabetes.
Q2: What are main signs of insulin resistance?
Signs include increased abdominal fat, constant hunger and sugar cravings, fatigue especially after meals, difficulty losing weight despite calorie restriction, dark skin patches on neck/armpits, and fasting blood sugar above 100 or post-meal above 140. Multiple symptoms together suggest insulin resistance requiring blood sugar control intervention through diet and lifestyle.
Q3: What should Indians eat for insulin sensitivity?
Eat adequate protein (80-100g daily), non-starchy vegetables unlimited, healthy fats from nuts and seeds, whole grains in controlled portions (1/2 katori brown rice/millets), legumes providing protein and fiber. Minimize white rice, refined wheat, sugar, sugary drinks, and processed foods supporting glucose stability through strategic insulin balancing diet.
Q4: Can insulin resistance be reversed naturally?
Yes, through insulin resistance diet emphasizing protein, fiber, healthy fats, limited low-glycemic carbs, plus regular exercise, adequate sleep, and stress management. Studies show 70% of prediabetes cases reverse with aggressive lifestyle intervention. Weight loss of 5-10% significantly improves insulin sensitivity within 8-12 weeks of consistent implementation.
Q5: How long does improving insulin sensitivity take?
Blood sugar improvements appear within 2-4 weeks of appropriate prediabetes diet changes. Significant insulin sensitivity improvement shows within 8-12 weeks of consistent nutrition, exercise, sleep, and stress management. Complete reversal of prediabetes typically requires 6-12 months sustained lifestyle changes preventing progression to diabetes.
Conclusion
Insulin balancing diet addresses root cause of weight gain, diabetes risk, and energy instability affecting millions of Indians through genetic vulnerability and high-carb dietary patterns. Strategic nutrition emphasizing adequate protein, controlled low-glycemic carbs, fiber, and healthy fats combined with regular movement, sleep, and stress management dramatically improves insulin sensitivity and blood sugar control. For Indians with prediabetes or insulin resistance, aggressive dietary intervention reverses condition in 70% of cases preventing diabetes development that would require lifelong medication and create serious complications.
Start this week by reducing refined carbs, replacing white rice with brown rice or millets in half portions, and adding protein to every meal. Monitor blood sugar 2 hours after meals learning your individual responses. Move after meals and prioritize 7-8 hours sleep. These foundational changes improve insulin function within weeks, creating energy, easier weight loss, and disease prevention.